The CDC has extremely strict rules for breast milk. It can be left out for four hours at room temperature, four days in the fridge, or up to 12 months in the freezer. You should never refreeze it once it has defrosted. You should never mix multiple temperatures of breast milk together (i.e., do not add warm milk to cooled milk). And if you start a bottle, you must use the rest within one to two hours. If you don’t, you should throw it away.
It’s possible that in an ideal world, with unlimited milk supplies and no logistical problems, these regulations might be easily followed. But in the real world — where milk spills, freezers are left open, and babies don’t finish their bottles — there are a lot more gray areas.
What’s the actual data behind storage times, mixing, and reusing a partially used bottle? What if I (heaven forbid) put the bottle back in the fridge and fed my kid again with it four hours later? What would actually happen?
Here’s the data on breast milk storage: when you can be flexible with it and when you should err on the side of caution.

The underlying concern: bacteria
Underlying all these CDC rules is a concern about bacteria. Breast milk, like all substances, has bacteria in it. These can come from the breast, from the air, from handling, etc. If the bacteria are pathogenic (say, something like staphylococci) and if they multiply to high-enough levels, they could make your baby sick. It is important to note that levels matter here. There are bacteria everywhere and in everything, even some bad bacteria. At low levels, that’s OK. At high levels, however, you have to be careful, and there are guidelines about how high these bacterial levels can be before they cause a problem.
Generally, freshly pumped breast milk has low levels of bacteria — far lower than any level that could cause an issue. But when breast milk is stored, bacteria have a chance to multiply. This growth is even faster at higher temperatures. It is widely understood and accepted that if you left breast milk out on the counter in the summer for four days, it would be spoiled. It would smell bad, taste bad, and possibly be dangerous. It’s also widely accepted that leaving it out for an hour is fine.
The question, on all of these exposures, is where the line is. So, what does the data say? Are these CDC guidelines necessary to keep bacterial growth low enough to be safe?
How long can breast milk be left out or stored in the fridge?
Since we can study breast milk directly, this question is answerable. The answer is necessarily going to depend on the temperature of the room. Bacteria grow more quickly when it’s hotter.
Earlier research on this question took samples of milk from 16 women and studied their bacterial growth at varying temperatures and timeframes, up to 24 hours. In this data, the researchers showed that at a temperature of 59 F, there was minimal bacterial growth by 24 hours. At 77 F, though, the minimal growth was maintained for only four to eight hours. At 100 F, even four hours saw considerable growth.
This suggested that even in a hot room, a period of storage in the range of four to eight hours would be acceptable. Similar data from Nigeria showed that storage for nine hours in tropical conditions (i.e., left out) did not generate bacterial loads that exceeded acceptable levels.
A new study actually takes this even further. (Fun fact: The study was funded in part by ParentData readers who were tired of waiting for this question to be answered!) Researchers in Germany took 44 infants (17 breastfed, 27 formula-fed), collected milk from them, and systematically measured bacterial growth at varying temperatures and time points, both before and after the baby fed from the bottle.
The results for pumped milk before feeding are striking: Bacterial growth was essentially flat at refrigerator temperature over 24 hours — which is not surprising. More surprisingly, bacterial growth was also negligible at room temperature over 24 hours. This means if you accidentally leave pumped milk on the counter overnight, you may not need to throw it away.
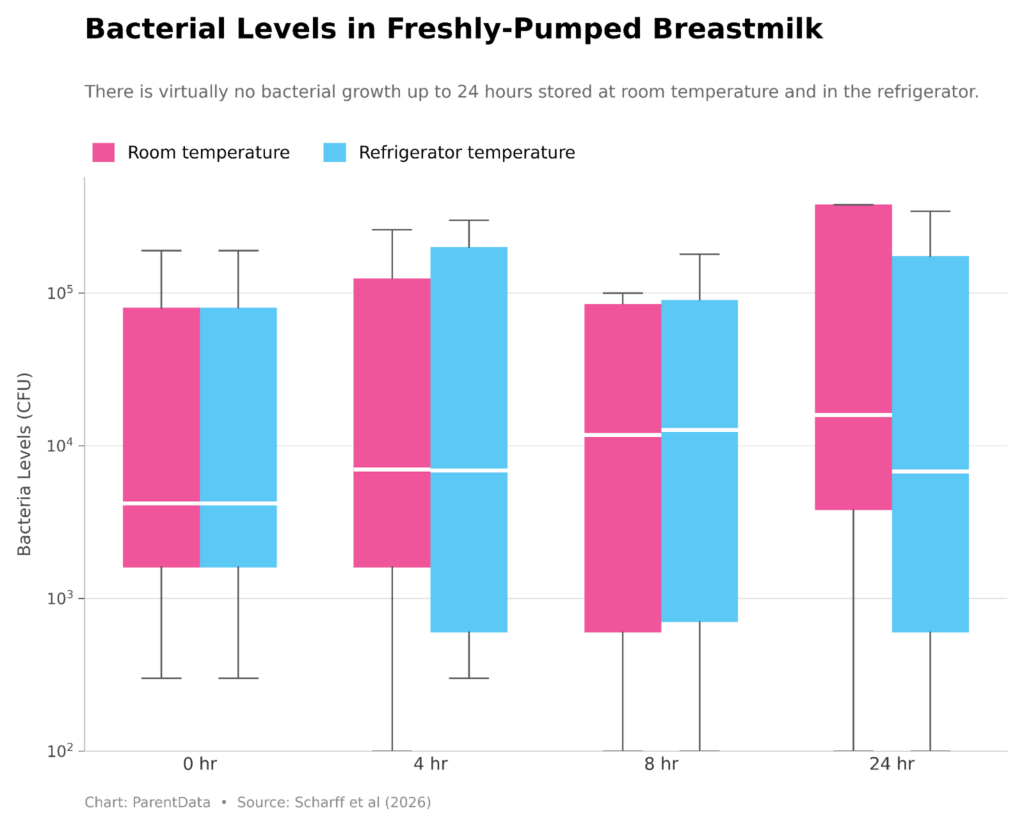
(It is important to say that the authors are primarily interested here in the growth of bacteria rather than the exact levels. When a baby drinks from a bottle, bacteria will transfer — we all have a lot of bacteria in our mouths all the time. This means that as soon as the baby drinks from the bottle, there will be sizable bacterial counts. The worry is that these counts might grow fast over time, which could pose a problem. If the count stays the same for many hours, even if it started out high, there is no reason to think that there’s a problem.)
At refrigerator temperatures, storage time can be considerably longer. This review article points to no appreciable bacterial growth at four days of storage at typical fridge temperatures. In the freezer, measurements at nine months show no indication of bacterial growth. Generally, the concerns with long-term freezing are due to a slow decline of vitamins, as well as the fact that the breast milk’s taste is eventually affected.
We can put this together to think about questions like what if I heated the milk and then put it back in the fridge? Bacteria would grow slightly more quickly during the heated period and then slow down in the fridge. Overall, the storage timing would be similar to what it would be if you just had it in the fridge, maybe a bit shorter.
What we have from this literature is a sense that over some reasonable period (several hours left out, at least several days in the fridge), breast milk bacterial levels are stable. What we do not have is much of a sense about the limits of this “reasonable period.” In the studies of the refrigerated milk, we see little bacterial growth at four days. Does this mean eight days is fine? Twelve? Longer-term analysis of the question where is the limit? is missing.
Can I refreeze breast milk if it thaws?
This question is especially important, in my view, because sometimes breast milk thaws by accident. I’ve heard from many people asking what they should do if someone in the house left the freezer door open and the milk defrosted overnight. And if you lose power after a hurricane or other major weather event, what happens to the milk in the freezer?
This is a question that can be studied using donor milk in carefully controlled conditions, as in this 2006 paper. The authors look at both bacterial load (a measure of pathogens) and vitamin and fatty acid content in milk treated in various ways. In addition to their analysis of storage without freezing, they also consider what happens if you take milk that’s frozen, thaw it, and refreeze it.
The frozen-thawed-frozen milk does not show an appreciable bacterial load; it is an order of magnitude lower than the FDA limits. A 2016 review article draws broadly similar conclusions.
There is some human judgment here; if the freezer is left open while you’re on a two-week-long trip, you do not want to refreeze the milk. But if it’s open overnight and everything thaws a bit, there is nothing in the data that would suggest you need to throw it away. Just close the freezer and try to move on. If you are not sure how long the freezer has been open or off, you can feel whether the milk is still cold or see if there are still ice crystals. If it is still cold, close it up. If the milk is room temperature, and it could have been many days, you may have to throw it away.
Can I mix multiple temperatures of breast milk?
If you are like me, you are not a prolific breast milk producer. I used 4-ounce bottles when I pumped, but I was never actually producing that much at once. Sometimes, there would be half-filled bottles. Was it OK to combine the new 2 ounces, still warm, with the older milk?
The guidelines say no. Many people wonder why. The simple reason is that the new milk will warm up the cold milk. When breast milk is warmer, it’s more susceptible to bacterial growth. However, we established above that, generally, breast milk is quite stable, and storage, even at room temperature, is safe for a fairly long time. Adding breast milk to a bottle — that is, slightly warming it for a brief period, while also leaving it in the refrigerator — is a very small change.
Put differently, if you think of yourself as having six to eight hours of room-temperature storage before you get concerned, the briefly warmer period while the milk comes to the same temperature can be counted against this amount of time. All in all, this risk is theoretical at best. You can mix without worrying most of the time.
Can I reuse breast milk after already having used some?
This is in many ways the most interesting question. When your baby drinks from a bottle, bacteria from their mouth get into the milk. For this reason, the baseline bacterial load will be higher right after they’ve drunk the milk compared with right before. The larger bacterial load will mean, of course, more possibilities for bacterial multiplication. This is why the CDC recommends throwing the milk away.
On the other hand, this is also the most interesting question from the standpoint of your life. It’s really, really frustrating to throw away pumped milk.
When I went looking for evidence about this, the first thing I found was evidence on formula. There are at least two studies (here and here) that had adults drink baby formula and then measured the bacterial content of the formula after drinking and after storage. In these cases, even after up to 24 hours of storage in the fridge, the samples did not produce high bacterial levels.
This is encouraging, but it’s about formula and not breast milk. However, we have other evidence that breast milk is much less prone to bacterial growth than formula. Putting these facts together, we would rationally conclude that the safe storage time of partially drunk breast milk might be higher than partially drunk formula.
A new study directly addresses this. After infants were fed from a bottle, the researchers stored the partially used milk and tested bacterial levels at four, eight, and 24 hours — both refrigerated and at room temperature. Their findings are reassuring. When refrigerated, bacterial levels after feeding were stable at four, eight, and 24 hours — growth was negligible. Even at room temperature, bacterial levels were stable at four hours and remained below levels of clinical concern at eight hours. The 24-hour room-temperature result showed slightly more variation, but was still not statistically significant.
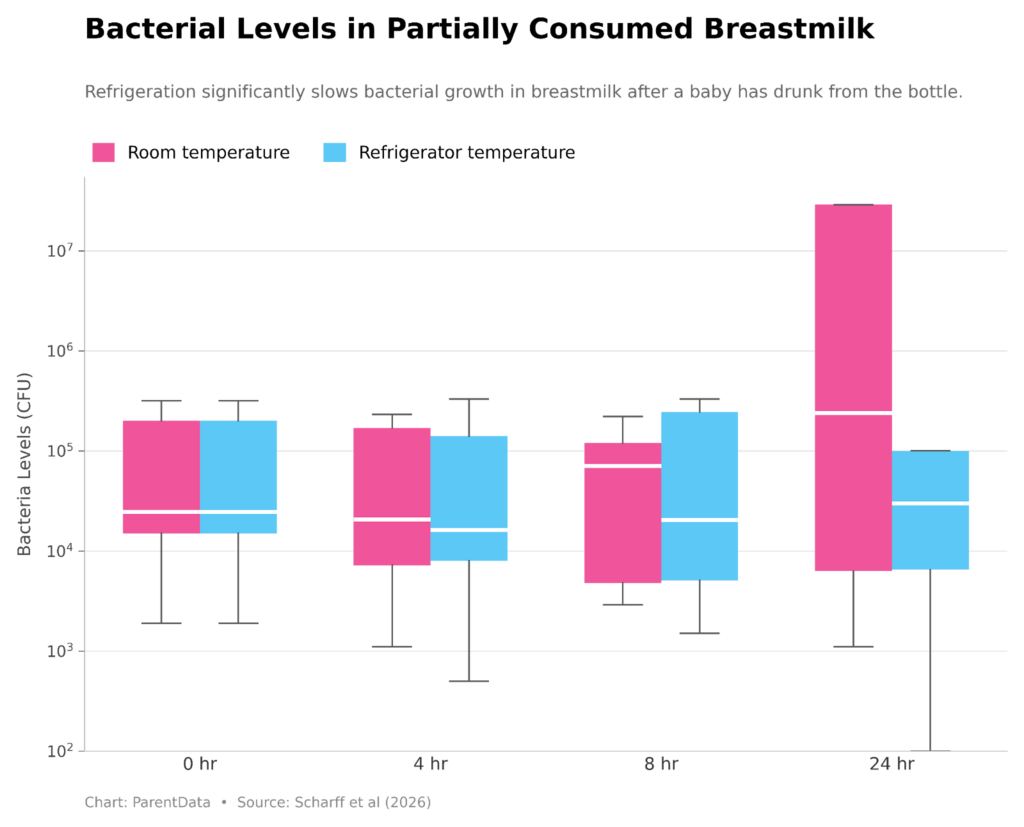
For context, this is meaningful because we previously had almost no direct data on this question for breast milk. The best evidence we had was a single unpublished undergraduate thesis from 1998, which was actually quite well-designed, but included six women and was not a professional study. We now have something substantially better.
On top of the logic, I would personally be comfortable storing partially used breast milk in the fridge for a reasonable period (and I did).
Closing thoughts
It’s important to note that there are some situations where we must be extremely careful about pathogens in milk. This includes when a baby is preterm, when the NICU is involved, and when we are discussing donor milk.
But for healthy babies, the guidelines issued by the CDC seem to be overly cautious in terms of the actual evidence on bacterial growth in breast milk. Breast milk appears, based on what we know, to be far more stable than guidelines suggest. Putting this all together, here’s where we land:

That said, while new research is emerging, science moves slowly, and no single paper is the final word. Many questions also remain open: What happens when you reheat milk that’s already been partially used and refrigerated? What are the outer limits of safe storage beyond 24 hours? More replication and more data are needed.
In the meantime, a reasonable person might ask why not just stay ultraconservative? The answer is that it’s annoying and costly. Pumping is hard. Throwing away milk that didn’t need to be thrown away is a real waste — in time, in effort, in money for those who supplement. The evidence we now have suggests that the stricter guidelines don’t seem to make your baby safer, and that matters.
The bottom line
- Freshly pumped milk has low levels of bacteria. The bacteria multiply when stored and multiply faster when it’s hotter. Even so, bacterial levels remain stable in unused breastmilk over a reasonable period — likely up to 24 hours at room temperature or several days in the fridge.
- It is fine to refrigerate partially used breast milk and reuse it within 24 hours, or up to eight hours at room temperature.
- Milk that has been thawed and refrozen does not show an appreciable bacterial load. If you accidentally leave the freezer door open overnight, you don’t necessarily have to throw the milk away.
- Mixing milk (adding new breast milk to a half-filled bottle and then returning it to the fridge) does not pose a risk of dangerous bacterial growth.
- When a baby is preterm, when the NICU is involved, or when donor milk is used, consult your pediatrician for the best guidelines to follow.



















Log in
Hi! What about once you’ve mixed formula with breastmilk? How long can you use this mix if it’s in the refrigerator and baby hasn’t touched it?
Can you combine breast milk pumped on different days? Can you combine frozen breast milk from different days?
Noting that the new study referenced here has not yet been peer reviewed- Emily, any sense of when that might happen?
I believe the authors are submitting soon — jounal timing is a little unpredictable.
Are there any studies about this in the works? How can we donate dollars or volunteer as breastfeeding moms? Together we can make a difference!!
Can already used milk be re-heated after being refrigerated again?
This was my question as well!
Also mine! For the babies like mine who refuse milk below body temp
One way to freeze just an ounce at a time without it being annoying is to buy a silicon freezer tray where each slot is an ounce or half ounce. Haakka & Souper Trays are great. You can then pop out the frozen cubes and still store them in small breastmilk bags or a larger ziplock one. The cubes are also are easier to put in bottles instead of waiting for the bag to thaw and hope you don’t spill pouring it into the bottles.
My first baby I did the one ounce square cubes but they were a bit harder to put into the small milk bags or narrow bottles. Second baby I’m doing half ounce round cubes and they’re def more versatile.
Great information! Does surrogate-provided milk fall into the same category as donor? Is the differentiation actually between breastfed breastmilk and pumped? And how is donor different? Thank you!
Thank you so much for this. Hopefully one day we can have the data to finally put people’s minds at ease but this has been my general approach for all my kids, whether it was formula or breast milk ( with both i would put unfinished milk in the fridge and use at the next feeding). My sense is that CDC and FDA guidelines are usually an order of magnetic lower/higher than thresholds where there’s actual evidence of adverse effects but we need more studies here! I remember years ago hearing my aunt express frustration because my cousin would toss formula that had been out for 61 minutes!