Of the many childhood illnesses, ear infections are the ones I remember getting most often. Every time, my mom would truck me off to our pediatrician, Dr. Morrison, who would dutifully examine my ears and prescribe me Bactrim (fun fact: I’m allergic to all drugs ending in -cillin and -mycin, so the standard first line of penicillin was off-limits). I’d take it, and 24 hours later I’d be better. Rinse and repeat a few months later.
For those of us with kids now, unless your child has very unusual ears, you’ve probably also experienced an ear infection or two (or 15). The protocol now, though, is a bit different. Often when I bring a child with an ear infection to the doctor, I’ll be given a choice — antibiotics or not — or, in some cases, prescribed antibiotics but told we can wait 24 hours to see if things improve on their own.
Why the change? Broadly, it reflects a combination of the fact that many or most ear infections resolve on their own and the fact that overuse of antibiotics is a factor in generating antibiotic-resistant bacteria. But it’s not a universally accepted change, and the somewhat confusing messaging that one often gets from a doctor (“you can wait, or not”) reflects this.
To try to cut through the confusion, today I’ll do ear infections. First, a quick primer on what they are. Second, the antibiotic-or-not question. Third, a discussion of what else you might do to prevent them (e.g. snot sucking).
A note: When kids get very frequent ear infections, especially younger kids, the question of ear tubes may come up.
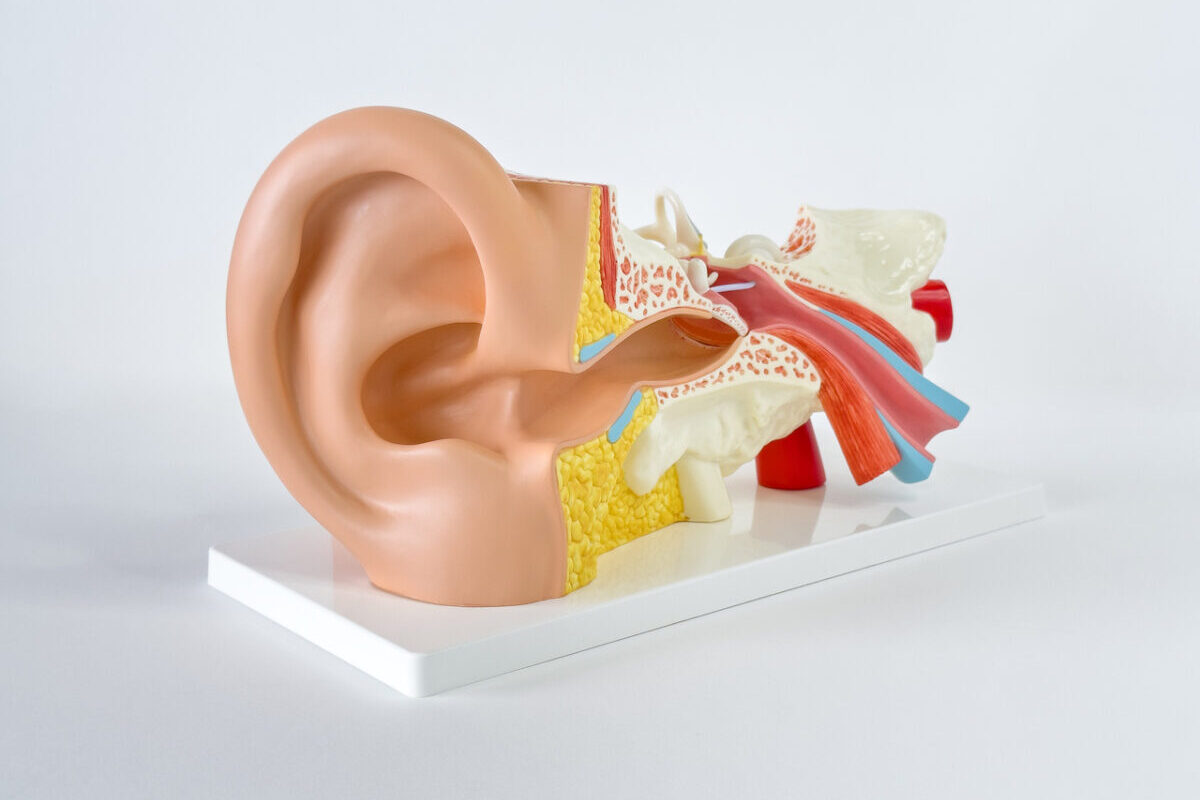
What is an ear infection?
It’s pretty simple. An ear infection occurs when fluid fills the narrow tubes that go from the ear to the back of the throat — usually but not always because of a respiratory infection — and then that fluid grows bacteria. The bacterial growth causes swelling and pain. Most ear infections (over 90%) in children will go away on their own eventually without treatment. Serious complications — mainly, eardrum rupture — can occur, although this is rare.
Ear infections commonly occur after a cold because the cold produces the fluid that builds up in the tubes. They are more common in children than adults because the smaller tubes are more likely to become blocked (and also perhaps because adults are better able to clear mucus; see section on snot sucking below). There is variation across kids in frequency, both because of variation in overall illness and because of variation in ear tube size.
Should ear infections be treated with antibiotics?
When I was a kid, it wasn’t just ear infections that got antibiotics. It was anything. In particular, upper respiratory infections (i.e. colds) were often treated with antibiotics. This was a mistake. Most of these illnesses are caused by viruses. Viruses are not killed by antibiotics, so this doesn’t make sense medically. And there are downsides to using antibiotics if they are unnecessary, including (from an individual standpoint) digestive issues and (from a societal standpoint) some contribution to antibiotic resistance.
Before moving to ear infections, let me underscore this point, since it’s a place where one’s own parents often seem resistant and confused. Yes, as a child, you probably got antibiotics for a cold. And sometimes that probably did make you feel better, since they reduce inflammation, which can improve some symptoms. However, if your child has a viral infection, antibiotics will not make them better. You should keep them hydrated, treat a fever if necessary with Tylenol or ibuprofen, and look for help if your child seems really sick. Viral infections are generally self-limiting. Despite what your mother-in-law says, antibiotics are not necessary.
Ear infections are a slightly different beast. Although it is usually a viral infection that causes the fluid to build up, the infection in the ear is generally caused by bacteria. As a result, antibiotics can help. However, your body is able to fight off some bacterial infections on its own, and in nearly all cases, ear infections in kids will eventually self-resolve.
This tension is why prescribing guidelines are a bit unclear.
One school of thought is that kids with ear infections should be prescribed antibiotics immediately, because this will make them feel better sooner. A second is that it is a good idea to wait, because the infection will likely go away on its own, and less use of antibiotics is better than more. Both of these positions have merit.
The case for less prescriptions: In a meta-analysis of settings in which children did not receive antibiotics, 50% of ear infections resolved within three days, and 90% within seven to eight days. During the COVID-19 pandemic, prescription treatment for ear infections went down a lot, without any increase in follow-on complications. On the antibiotic-resistance side, although it is extremely difficult to make statements like “one more prescription has this impact on resistance,” there is data suggesting that countries in Europe with more general antibiotic prescribing have higher rates of resistant bacteria.
The case for prescribing now: The case for prescribing antibiotics to kids for ear infections is that they do seem to get better faster. In a Cochrane review of studies that compared antibiotic treatment with placebo, the authors found that antibiotics reduced pain at three days (16% versus 11%), and also at a week and 10 to 12 days. Basically, kids got better faster with the antibiotics, on average.
With these competing viewpoints, one interesting way to look at the data is to ask what doctors do when it comes to their own families. If you were a medical professional, would you use antibiotics on your own kids?
A recent paper by several economists looks at this very question in Swedish administrative data. [Full disclosure, my husband is one of the authors on this paper.] The authors here are able to link individuals to both their prescriptions and also their family’s professional background, to look at questions like “When the family includes a doctor, are they more or less likely to adhere to standard prescribing guidelines?” The paper asks this question in a variety of settings. Most relevant for this post, they look at adherence to the guideline that children should be prescribed narrow- rather than broad-spectrum antibiotics.
I will note that this is not precisely the same question we are asking here, but it’s closely related — they ask whether families with medical professionals treat infections with more or less aggressive measures. The answer is more aggressive. Across nearly all settings, but especially in antibiotic treatment for children, families with doctors in them are more likely to use more aggressive treatment that goes against the standard guidelines.
Does this mean you should treat your child with an ear infection with antibiotics? Not necessarily! It’s just one (interesting) piece of data.
Putting this all together, though, you can see the argument for the wait-and-see approach. In the Cochrane review of antibiotics treatment versus not, they find that 60% of ear infections resolve at 24 hours regardless of treatment approach. Where they see differences in antibiotics versus not is in the longer time frame. This works in favor of an argument to wait a day, see if you’re in the 60%, and treat if not. Of course, that’s another day of missed school and work if you guessed wrong.
There is no easy answer to this! My goal with this discussion is to at least help you understand the tradeoffs.
Is there any way to prevent ear infections?
Obviously one way to prevent ear infections is to prevent colds. But if you have kids, that’s not really possible. If they do get a cold, can you do anything to avoid ear infections?
In principle, reducing the amount of mucus in their nose could help. Less fluid buildup equals less opportunity for bacteria to grow.
Kids, and especially babies, often cannot blow their nose well, so if you want to accomplish this, you’ll need to do it for them with a snot sucker, like a bulb syringe or a NoseFrida or (for older children) a nasal wash. The idea with all of these options is to clear out the nasal cavity, more effectively and gently than with nose blowing.
Do these actually reduce the risk of ear infection? There isn’t much concrete evidence. One Italian trial found some reduction in ear infections, but the data is fairly weak. Any claim that these work must be largely based on the mechanistic theory — which is there, but doesn’t tell us if this works in practice.
There are other possible reasons to use a snot sucker on your baby or small child, most notably that they may feel more comfortable and sleep better if they are less congested. If it seems like it helps your child, great. But the data definitely doesn’t guarantee fewer ear infections.
Community Guidelines



















Log in