During labor, your baby’s heart rate will be monitored throughout to ensure they aren’t in any distress.
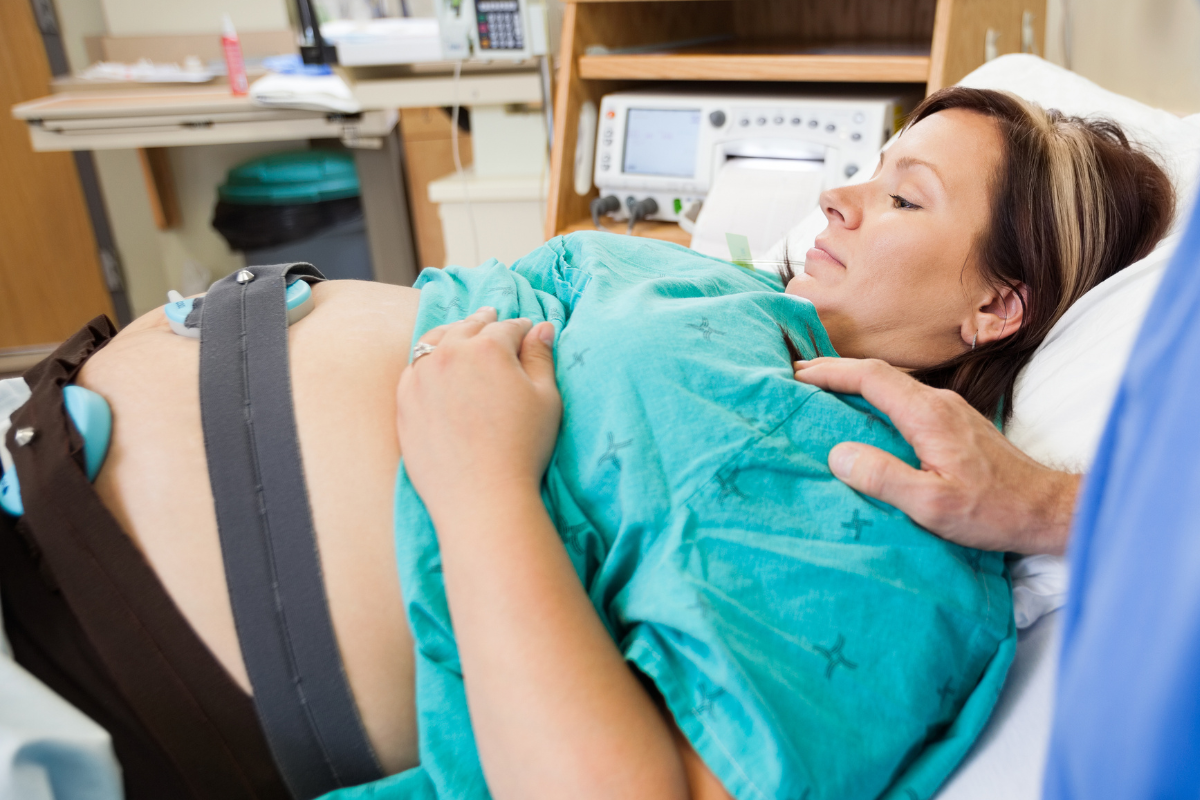
In the U.S., it’s extremely common to have continuous fetal monitoring — that is, a continuous record of the baby’s heart rate and your uterine contractions. This is usually done by placing elastic bands around the belly with electric sensors. However, intermittent monitoring, which involves checking the heart rate every 10–15 minutes with a Doppler, is sometimes preferred for low-risk pregnancies. While in principle intermittent monitoring seems like it might be better, the data in practice is more complex.
Continuous fetal monitoring was first introduced in the 1960s with the goal of better monitoring babies during labor and preventing bad outcomes. But is it the right choice for all pregnancies?
What are the benefits of continuous fetal monitoring?
A 2017 Cochrane Review pooled data from 13 randomized controlled trials with over 37,000 women — including both low- and high-risk pregnancies — comparing continuous monitoring with the intermittent alternative. The primary outcomes they were looking for were changes in neonatal seizures, perinatal mortality, and cerebral palsy rates.
The review did not find lower rates of mortality or cerebral palsy (often a consequence of issues during birth) for births with continuous monitoring. The authors did find that continuous monitoring was associated with a very small reduction in seizures — based on their estimate, this might reduce seizures by 1 in 1,000 births.
This data is largely based on quite old trials, many of them run in the 1980s. That should give us pause in general, since technology has advanced quite a lot since that period. More recent evidence is somewhat limited, although it shows broadly similar results. A 2018 study of over 3,000 women in Ireland found no difference in neonatal outcomes between continuous and intermittent monitoring.
There is also some evaluation of continuous monitoring with and without a computer-aided decision tool (which, ideally, would help doctors react more effectively to the information). The main trial of this also shows no difference in infant outcomes.
The overall picture is of fairly minimal benefits from continuous monitoring. For people whose infants are at higher risk of seizure — those with preeclampsia, gestational diabetes, or other complications — these benefits may be higher.
What are the risks?
There are two primary concerns with continuous fetal monitoring. One is that it can be physically constraining if you are hoping to be mobile during labor — the bands can move off of your belly as you move around, cause alerts, and need to be repositioned. This is more about experience than safety, but experience matters, so it is worth saying.
The second concern is that this continuous monitoring could lead to a higher risk of a C-section.
In the 2017 Cochrane review, the use of continuous fetal monitoring raised the chance of having a C-section by 63%. This is a significant increase and — combined with the fact that outcomes were largely unchanged — it suggests that the additional C-sections did not provide benefits. Having access to a C-section if needed is absolutely essential during labor, but it should only be used if necessary, and this data suggests that continuous monitoring leads to more unnecessary C-sections.
Again, the review mostly includes older data, and in the randomized trial published in 2018, the authors found no difference in C-section rates. This could reflect a different population, a better understanding of how to read the data, or something else. It is hard to know.
Is continuous fetal monitoring necessary?
The American College of Obstetricians and Gynecologists (ACOG) endorses intermittent monitoring as an alternative to continuous monitoring for low-risk women. Indeed, their opinion suggests hospitals should improve their training on how to do this, so it is an option for people who want it. Best practice here is that this should be a choice made by patients and their providers.
If you have a high-risk pregnancy, there is a more compelling argument for continuous monitoring. If you have a low-risk pregnancy, you likely have more options. These are worth discussing with your provider, since for many women, there may be a strong argument against the continuous approach and only a very weak argument for it.
The bottom line
- Continuous fetal monitoring reduces neonatal seizures by a very small amount (roughly 1 in 1,000 births) and has not been shown to reduce mortality or cerebral palsy rates.
- The trade-off is real: continuous monitoring significantly increases the chance of a C-section, without improving outcomes.
- For high-risk pregnancies, continuous monitoring makes sense. For low-risk pregnancies, intermittent monitoring is a legitimate option endorsed by ACOG — and worth discussing with your provider before you’re in the room.




















Log in