Mastitis. If you’ve had it, the word itself prompts a reaction. When I mentioned the topic in our ParentData Slack channel, one team member commented, “Just the thought of this gives me a fever.”
For those who have no idea what I am talking about, here’s a quick overview. Mastitis, in general, refers to a condition in which the breast is swollen, hot, and painful. It can occur outside of breastfeeding but is most common during that period, when it’s referred to as “lactational mastitis.” Lactational mastitis occurs in something between 2% and 20% of breastfeeding people and is part of a much larger continuum of related discomforts.
But while mastitis is a common experience among people who breastfeed (or at least something they’re aware of), the guidelines about how to treat it are confusing and differ depending on who you ask. So, what is the best way to treat it? And, more importantly, why is this question so hard to answer?

How does mastitis start?
Mastitis often starts with a combination of an oversupply of milk and bacterial growth. When we talk about an “oversupply,” we simply mean that there is more milk than the baby needs; you may realize you have this if your breasts still feel full after a feeding or are full and uncomfortable long before your baby is ready to eat.
Oversupply of milk can occur for various reasons; it is common in the early weeks of breastfeeding, during weaning, or at any time when the cadence of nursing changes, and your supply needs to adjust (your baby starts sleeping through the night, for example). The oversupply can lead to milk stagnating in the breast, which may cause bacterial growth. The excess bacteria and milk can lead to a narrowing of the milk ducts, which can then progress to inflammatory mastitis. That can then advance to bacterial mastitis or (rarely) to abscess.
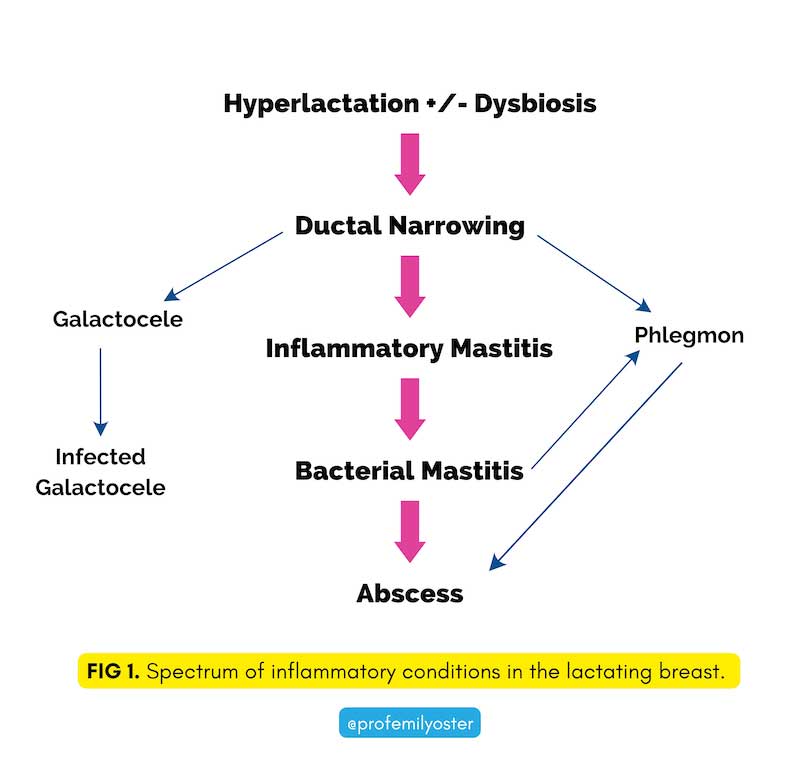
When mastitis progresses to the later stages, it can lead to systemic symptoms, including fever and fatigue. In these cases, there is widespread agreement that it is necessary to treat it with antibiotics, and antibiotic treatment is effective in nearly all cases. It is also completely fine to continue to nurse while on antibiotics.
Important note: Please do not be anxious or reluctant to ask your doctor about this. Do not just suffer in silence!
What are the guidelines for treating mastitis?
In early stages, mastitis can and often does resolve on its own, and early on, it may be possible to reverse course. To enhance that possibility, the breastfeeding person is typically prescribed what we might call “supportive care.”
We can divide this advice into two parts. The first is what we might call the “nonspecific” or “obvious” part. This includes advice like “drink fluids and rest” (easy to say, harder to do with a baby), take ibuprofen or Tylenol for pain, and avoid wearing tight compressive bras (like sports bras).
The second is advice that is more distinct to the breast. Historically, there have been four key recommendations:
- Apply warm compresses to the breast or take a warm shower.
- Breastfeed frequently, starting with the affected breast.
- Use a pump to express milk between feedings.
- Massage the breast area.
This was the standard advice until 2022. In that year, the Academy of Breastfeeding Medicine came out with new guidelines, which largely said the opposite. Here is my summary of their version:
- Apply ice to the breast. Warm compresses might make things worse.
- Continue to breastfeed, but do not favor the affected breast; in some cases, use only the unaffected breast.
- Minimize breast pump usage; do not “pump to empty” the breasts.
- Avoid deep massage of the breasts.
With such a dramatic change in advice, it is natural to wonder what changed; what new evidence came out to support this? The short answer is that neither the old advice nor the new advice is especially well grounded in concrete evidence.
For example, in the 2022 guidelines, the authors state: “The use of warm showers and antipyretics [fever-reducing medications] did not improve mastitis outcomes in a randomized controlled trial.” This statement seemed quite compelling to me and is perhaps the strongest direct refutation of the older advice. When I went to the citations for this claim, though, I found a randomized trial of acupuncture for the treatment of mastitis. The trial rejected the value of acupuncture, but I didn’t see anything on showers.
Searching through the text, I found the evidence in support of the warm shower claim. One of the groups took more warm showers than the others and didn’t have their mastitis resolve any more quickly. This is weak evidence — it certainly isn’t randomized — and the samples in this paper are small (200 women in total over three treatment groups).
In practice, the arguments in favor of the updated guidelines are largely based on logic and what we know from other contexts.
Which mastitis guidelines should I follow?
Mastitis is part of a continuum that often begins with an oversupply of milk and ductal inflammation. The logic in the most recent guidelines from ABM is simple: if you want to address the problem, you need to address these causes. This means downregulating supply, especially from the affected breast, and reducing inflammation. It is these observations, rather than experimental data, that point to the conclusions.
Hot versus cold for treating mastitis
Any topical temperature change on the breast would be designed to treat inflammation. In general, inflammation is more often treated with ice rather than heat. This is a generic statement about all inflammation (it’s why athletes like ice baths), but we can see why it would apply here, too. If you want to treat inflammation, ice is the initial go-to choice. If you do not want to put ice directly in your shirt, there are breast-specific cold packs.
Which breast to begin with? Should you pump or not?
The advice about which breast to start on and whether to pump is intimately related to the issues of oversupply.
Many cases of mastitis are a result of oversupply, so treating it will involve lowering the supply. Breast milk supply responds to demand. If you nurse and pump more in general, your body learns you need to produce more milk and makes more of it. Similarly, if you nurse and pump more on one side, that side will be more active. This is something you may be familiar with if your child has a favored breast. One of my kids vastly preferred to nurse on the right side, and it led to a very lopsided look (it mostly got better).
By extension of this theory, though, if you take a breast that already has an oversupply and you encourage more supply, you might make the problem worse. Much of the standard advice has this feature. Encouraging people to start nursing on the affected side will increase production on that side. Pumping between feedings, or “pumping to empty,” also generates more supply.
In contrast, starting nursing on the other side and avoiding or limiting the use of the pump will help the breast regulate. This is a bit of a balance. Especially with an engorged breast, completely ignoring it will also be very painful. An approach of “pumping (or hand-expressing) to comfort” (rather than to empty) may be a way to generate the right feedback without stimulating supply.
Massage for breast pain relief?
Massage is actually the trickiest part of this. There is general agreement that very light “sweeping” massage can be effective and relieve pain. However, in some cases, people will more aggressively massage in an effort to remove a perceived milk “plug.” This will not work, though. Mastitis isn’t caused by a particular stuck piece of milk in a tube. The breast has many, many ducts, and they get inflamed but not plugged up. As a result, aggressively massaging to remove a milk plug doesn’t make sense.
And, further, when you already have inflamed tissue, deep massage can possibly make things worse by increasing the inflammation and damaging the tissue.
Closing thoughts
Based on the logic of breasts and breastfeeding, the 2022 ABM guidelines make sense.
The most key and important seems to be the guidance on supply. If you take nothing else from this discussion, it should be that stimulating more supply in the affected breast is not a good idea.
Beyond that, what I took from this was a feeling of frustration. A huge share of breastfeeding people will experience some form of inflammation or mastitis during their breastfeeding journey. All of these people are looking for relief, and we should be giving them advice based on evidence. Despite this, the data is so limited that literally, people are getting the exact opposite advice, depending on who gives it.
My call to action here, then, is for someone to do a randomized trial. I do not think this would be all that hard. Recruit people with mastitis, randomize them into different protocols, and figure out if ice really works better than heat. Determine the right protocol to relieve engorgement without generating more oversupply. See if it is possible to improve knowledge about massage. I hope someone will do this. If you need help recruiting a sample, please let me know.
The bottom line
- Mastitis treatment guidelines changed in 2022 (now recommending ice over heat, less pumping, limited massage), but neither the old nor new advice is backed by solid research—just logical reasoning about reducing inflammation and milk supply.
- The key principle: avoid stimulating more milk production in the affected breast by starting nursing on the unaffected side and only “pumping to comfort” rather than emptying completely.
- Deep massage to remove a “milk plug” doesn’t work and may worsen things, since mastitis involves inflamed ducts throughout the breast, not a single blockage.
- If you develop fever and fatigue, antibiotics are highly effective and safe while nursing—don’t hesitate to call your doctor.






















Log in
Currently on my second baby and my eighth clogged duct / mastitis experience. I totally support and understand the logic around inflammation, but to say there’s no “clog” feels wrong based on my experience. I’ve had milk blebs interfere with drainage from the nipple. I’ve also been able to feel clogs originating deeper in the breast pass through my nipple while nursing (big ouch), then magically the affected area can drain.
This article doesn’t touch on the lack of real data around sunflower lecithin, a commonly mentioned supplement that is supposed to help prevent clogs. This lack of data, I find very frustrating. It would not be hard to study efficacy in a placebo trial.
TLDR/ breast inflammation is terrible and why the heck don’t we have more real data?
It’s just anecdote, but I’ve found the new guidelines to be very effective and I never had clogs progress to mastitis, even when downregulating a significant oversupply and experiencing several clogs. I would take a big dose of ibuprofen as an anti-inflammatory about 30 minutes before I expected to feed and then use ice packs between feedings. My early days of breastfeeding my son involved a lot more massage at the recommendation of lactation consultants and I had much worse engorgement with him than I did in my daughter’s early days, where I exclusively used the new recommendations. And to the person asking about blocked ducts–they exist in the sense that a duct can become inflamed to the point that it is “blocked” but it’s not that a chunk of milk is blocking it, it’s that your ducts have narrowed due to the inflammation, making it more difficult for milk to pass through.
But what about cabbage leaves??!!!
I’m slightly confused by your massage-related comment about blockages – are you intending to say there’s no such thing at blocked ducts? Or just that this article is about generalised mastitis rather than mastitis specifically caused by a blocked duct?
One final thing – the (preventative) solution that finally solved my recurrent blocked ducts (if such things exist) and mastitis was advice on positioning from an IBCLC lactation consultant who identified that my nipple pointed ‘the wrong way’ so baby wasn’t draining a whole section of boob. Just leaving that here in case useful for others.
As always, Prof Oster thank you for diving into the evidence on an important topic. I recently ended my milk production journey prematurely due to recurrent (and relentless) inflammation which resulted in multiple rounds of mastitis. In the throws of being a postpartum first time mom, I found the conflicting evidence incredibly confusing and overwhelming. I hope more research into this topic will mean we can do better for others in the future.
Thanks for sharing this recap of the new recommendations, Emily! As someone who had one child before the new recommendations were approved, and one after, and mastitis early in both postpartum periods, the complete shift in recommendations was confusing and frustrating, to say the least. While as a researcher, I agree with the suggestion to do a true RCT and determine which pathway is better, I think there’s a big hurdle to overcome: willing participants. Mastitis often occurs in the early weeks postpartum, when the mother is trying to figure out how to be a mother for the first time, feed her baby, feed herself, etc; OR, she’s doing all of that except the first time part and trying to also care for another child/other children. I’ll admit, even as a researcher, if someone had asked me to participate in a clinical trial in either of those early-postpartum mastitis-ridden moments, I would have replied with an emphatic, “no, thank you.” But I’m only an “n” of 1. I’d love to hear what others think, and what you think may be alternatives to get around this hurdle.